It’s the last Friday in June and the pews of Saint Benedict’s Parish in Halifax are filled with people of all ages and walks of life who have one thing in common.
Each one of them has come to say a final farewell to a family member or a friend who donated their body for the advancement of medical education and research.
The soaring notes of soloist Anita Simmons-Clancy set the tone for a service that included a reading of the names and heartfelt eulogies from university students and a resident physician who benefitted from the body donations via their anatomy labs.
In a touching service that left many dabbing the corners of their eyes, the Human Body Donation Program paid tribute to 129 donors at its annual memorial service. The remains of donors typically remain in the program for anywhere between one to three years and the program’s capacity for acceptance each year is usually between 100 and 120 bodies.
The Human Body Donation Program is operated by the Dalhousie University’s Faculty of Medicine and the Department of Medical Neuroscience, and partners closely with the QEII Health Sciences Centre for teaching and education opportunities.
For many attendees at the memorial service, it is the first official service held for their loved one. One of those who donated his body for medical research was Ron Blom.
Sandi, Ron’s wife, attended the memorial service with her family. A passionate advocate of the program, she doesn’t regret for one second the decision she and her husband made.
“I highly recommend this. The loss of your loved one is so overwhelming but this experience with the Body Donation Program helped me keep my sanity,” Sandi says.
Sandi and Ron were teenage sweethearts, best friends and business partners. Ron suffered a severe stroke in 2011, and the couple moved from Ontario back to their home province of Nova Scotia in July 2012.
One of the first things Sandi did when she arrived in Halifax was contact the Human Body Donation Program.
“When my husband and I were living in Ontario, my stepdad passed away. Mom told us he was donating his body (to Dalhousie) and we found it fascinating as it was the first time we’d heard of it,” she recalls.
“When Ronnie did pass, his palliative care nurse came to our home and was a tremendous help; and when the people came for his body they were so quiet and professional and they looked after everything,” Sandi remembers.
Professional, empathetic, dedicated, kind. Those are all words used to describe Brenda Armstrong, coordinator of the Human Body Donation Program and the first point of contact for anyone exploring the possibility of donating their body for medical education and research.
The program currently has 60,000 to 70,000 potential donors on file from throughout the Maritimes. In addition to completing forms that are kept on file noting the individual’s intention to donate remains at the time of death, individuals need to inform their families of their decision.
“We also highly recommend that at the time of making their intention they also have an alternate or backup plan that could be followed because the decision to actually accept the remains is only made at the time of death and sometimes, unfortunately, circumstances do not allow for all remains to be accepted,” Brenda explains.
The number one reason for refusal of remains is if the program is closed, typically due to their facilities being full. Other reasons for refusal include issues that interfere with preservation of the remains--things like unhealed surgeries, major traumatic accidents and burns.
“Basically, remains are used for teaching purposes for students in many disciplines - medical and dental programs, occupational therapy, physiotherapy, and nursing,” explains Catherine Currell, the Human Body Donation Program’s department administrator and program manager.
“We also have learners through our Clinical Cadaver Program for the residency programs at the QEII which take place namely at the Skills Centre and that would be for teaching purposes at a higher level.”
An important extension of the Human Body Donation Program, the Clinical Cadaver Program has been in place since 2007. It provides a teaching and learning experience on specimens that are nearly indistinguishable from live patients.
“There are two types of embalming. One is traditional, which is generally used for our undergrad teaching programs, and then there’s our clinical, which really is a light embalming which makes the remains more lifelike,” Catherine explains.
“The Clinical Cadaver Program uses these remains at the QEII. Most of the sessions are done at the Skills Centre and the disciplines that use them range from orthopaedics to urology, neurology, the whole gamut, really.”
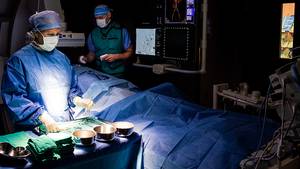
The Simulation Bay at the QEII’s Charles V. Keating Emergency and Trauma Centre also benefits from the Clinical Cadaver Program. Health professionals ranging from practicing physicians to nurses and paramedics can all train there on an ongoing basis, honing skills ranging from suturing to scopes and intubation.
“One paramedic can intubate a cadaver 20 times in a half hour. That’s equal to two years of field work,” explains Rob Sandeski, the Human Body Donation Program’s anatomical laboratories coordinator.
“You put that same opportunity in the hands of a skilled surgeon and patient safety rises ten-fold.”
In addition to increased patient safety, Rob says the QEII’s Clinical Cadaver Program increases the confidence of clinicians who can practice rare procedures they might not typically encounter.
“When you get into these clinical years, these skills are being honed and the benefits to the patients they care for are tremendous,” Rob says.
To learn more about the Human Body Donation Program, call 902 494 6850 or visit medical-neuroscience.medicine.dal.ca/donation.