Just outside your heart, where its final chamber meets the rest of your body, there stands the aortic valve, a gateway of fleshy flaps which ensures all your blood flows in the right direction. With each heartbeat this valve opens to let blood escape, but when the heart contracts, it closes to prevent any from flowing back in.
But for some of us, the passing of years allows a build up of calcium on this valve, holding it closed regardless of which direction the blood is flowing. The heart is an intelligent organ and pumps harder against this gate of cemented calcium, but eventually even this isn’t enough, and the body feels the pinch of inadequate blood flow.
Such was the case of Norman Thompson from Stratford, P.E.I. In June 2016, at the age of 90, he very suddenly traded his relatively active lifestyle for persistent exhaustion, as well as being unable to walk with ease, catch his breath or even enjoy a good night’s sleep.
“It was as if he’d just run a marathon and was out of energy,” says his wife, Ireta.
The calcification of one’s aortic valve is most common among the elderly, says interventional cardiologist Dr. Najaf Nadeem, especially among those over age 75. If untreated, half of patients can die within two years of showing symptoms, which include the aforementioned exhaustion, shortness of breath, heavy chest pains, passing out and even fatal arrhythmias. For a very long time, this condition’s only remedy has been surgery.
Dr. Christine Herman is a cardiovascular surgeon and colleague of Dr. Nadeem at the QEII. She says that calcified valves need to be replaced with artificial ones, made either of metal or animal tissue, and for this, surgeons must employ open-heart surgery. This requires the sawing of a patient’s sternum and the support of a heart-and-lung machine, says Dr. Herman, a procedure some patients are physically unable to endure.
Norman was far from an ideal candidate for something so invasive, given his age, but thanks to recent work at the QEII, open-heart surgery wasn’t his only option.
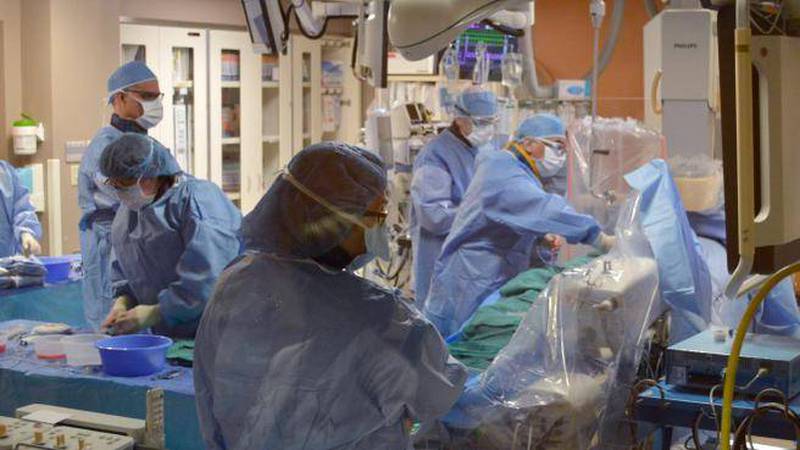
Transcatheter Aortic Valve Implantation, or TAVI, was first employed in France back in 2002 and is slowly becoming an adopted practice in Canada. In 2009 Dr. Nadeem helped establish the QEII’s own TAVI program, a multidisciplinary team bringing this promising procedure to their most at-risk patients.
Dr. Herman, herself a program member, says it does away with open-heart altogether. Instead TAVI calls for a small incision in the groin allowing surgeons to access the femoral artery, using it to feed a wire all the way back to the heart. Once in place, this wire serves to guide a catheter into the malfunctioning aortic valve, where it balloons to force the old valve aside. A new valve is then guided up the wire and expanded into place with the same ballooning action, where it remains fixed.
“The risk of death during TAVI is similar to those of traditional surgical procedures,” says Dr. Nadeem, “but it offers quicker recovery, a better initial quality of life and it’s much less invasive. There’s less risk of bleeding complications, kidney injury and irregular heartbeat.”
TAVI is very new to Canadian health care, as yet lacking the track record of open-heart surgery and costing considerably more, so for the time being it’s reserved for patients who need it most, Norman among them.
“He went into surgery looking terrible,” said Ireta, “but came back looking pink and bright, sharp as a tack. It was just amazing, from death to life.”
His procedure was carried out December 13, 2016, and unlike his counterparts enduring open-heart surgery, he returned to his Stratford home a few days later, December 17.
“You walk in, you get the procedure, you walk the same evening and then you go home the next day,” declares Dr. Nadeem.
Today, Norman is 91 and while he’s learning to take things in moderation, his heartbeat is as strong as ever.
Dr. Nadeem says that, of the 350 aortic valve surgeries they conduct in a year, roughly 60 will be TAVIs, but as the procedure continues to prove itself and costs drop, he fully expects it to become the surgery of choice.