Dr. Dave Padmore was desperate, dying and in need of a miracle.
Dr. Padmore is a urologist in Truro and a survivor of prostate cancer. When surgery did not remove all of the cancer, he opted for a combination of radiation and chemotherapy in the summer of 2012.
“By the time I finished in September, I was a wreck,” he says. “I had radiation effects in several parts of my body, but what made me most sick was radiation inflammation of my colon and rectum.”
It was a brutal, severe reaction. He lived in constant agony and says he could not function without pain medication.
“I could not work, eat, sit or even wear pants. It was not getting any better.”
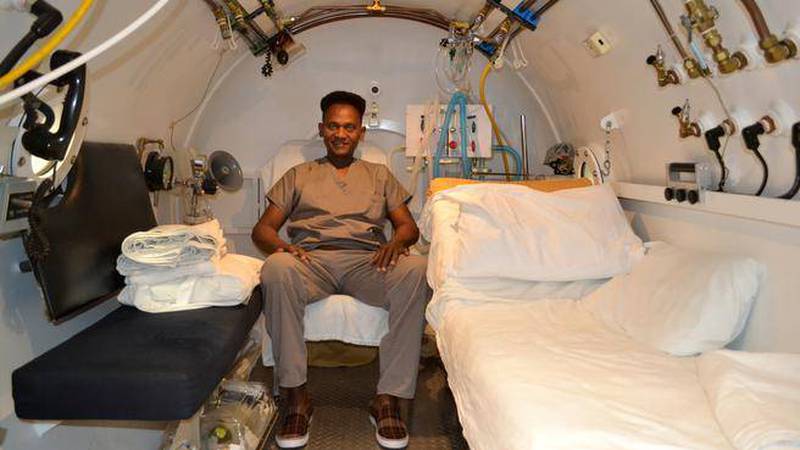
As a last effort, he turned to hyperbaric oxygen while he was home with his family in Barbados. He completed his final four weeks of hyperbaric treatment at the QEII, which houses the only hyperbaric chamber in the Maritimes.
For Dr. Padmore the effects were felt quickly.
“Within four weeks of starting, the light just lifted and the pain started to go.”
Hyperbaric therapy worked for Dr. Padmore as it has for many others with delayed radiation injuries. The blood vessels in these areas fall apart anywhere from six months to five years after radiation treatment. Cancer survivors with tissues that have been damaged by radiation make up 75 per cent of the patients treated in the chamber in Halifax.
Only hyperbaric medicine is able to grow a new blood supply for these patients.
“To me, it was nothing short of a miracle,” says Dr. Padmore, who recently completed a second round of eight-week hyperbaric treatment in Halifax, after more radiation damage caused internal bleeding in his bladder.
“I never felt in danger from my cancer. But when I was not eating, wasting away and in pain from radiation damage, this saved my life.”
It may seem miraculous, but it’s just science for Dr. Debbie Pestell, diving and hyperbaric medicine consultant at the QEII.
“When breathing 100 per cent oxygen under pressure, you force angiogenesis, which is the growth of new blood vessels,” says Dr. Pestell.
“We can grow new blood vessels on our own but it’s a slow process and if the wound is hypoxic, meaning it doesn’t have enough oxygen to it, it can’t grow the new blood vessels. It’s a vicious cycle because the way you get the oxygen is on hemoglobin through blood vessels.”
Generally, patients are treated daily for eight weeks in a hyperbaric chamber at the QEII’s VG site. The treatments are called dives, but patients never get wet and the chamber never actually moves; it is accomplished through changes to air pressure.
“In the chamber we compress the air. Based on research, most of our treatments go to 45 feet, then put the hoods on and patients breathe 100 per cent oxygen.”
Patients are monitored by a nurse or respiratory technician inside the chamber and are given intermittent breaks to breathe normal air in the chamber as well.
“So why does hyperbarics work?” she asks. “The excess oxygen goes into your plasma. Normally your body doesn’t need it, but if it’s in an area that is hypoxic, the body makes use of it.”
Hyperbaric oxygen forces the body to grow new blood vessels to promote healing and is a scientifically-proven treatment for 14 health conditions. The most common for Dr. Pestell at the QEII are complex non-healing wounds such as diabetic foot ulcers and delayed radiation injuries such as Dr. Padmore’s.
It is also used to treat failing skin grafts, carbon-monoxide poisoning, decompression sickness and even some burns.
The popularity of hyperbaric oxygen therapy is increasing as more doctors become educated on the science and more young doctors learn about it during their training.