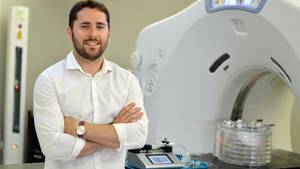
Ryan MacKenzie suffered his first seizure at the age of 18, dressed in formal attire and waiting, anxiously, for his prom date. He never did reach the dance floor.
Epilepsy occurs in one per cent of the global population, roughly 300,000 Canadians, of whom Ryan is one, living in Dominion, Nova Scotia. While this condition has a variety of causes, they all relate to an injury of, or developmental problem with, the brain. And even if seizures are the most obvious manifestation of epilepsy, they’re far from the only one.
Dr. Kristin Ikeda is a neurologist and epileptologist with the QEII Health Sciences Centre’s epilepsy care team. She says the modern definition of epilepsy goes above and beyond the occurrence of seizures, including depression, anxiety and sometimes even social and cognitive issues which can impact all aspects of a person’s life.
“It’s estimated 80 per cent of people with epilepsy will have some kind of cognitive issue severe enough to interfere with some aspect of their life,” she says.
Ryan, now 20, wakes up from seizures overcome by exhaustion. Socially active, employed and generally noted for a positive attitude, the uncertain timing of his next seizure still plagues him with understandable anxiety.
“I’m just living life and hoping for the best,” he says.
The treatment of epilepsy always begins with medication but as Dr. Ikeda describes it, only 50 per cent of patients will respond to the first medication they’re given. The odds with a second medication drop to 15 per cent and if continuing seizures oblige them to try a third, odds of success drop to less than five per cent.
The only remedy for “drug-resistant epilepsy” is to remove the portion of brain causing it, but of course this comes with risk. While speech and memory is typically stored by a person’s left brain hemisphere, some house these mental faculties in the right. Others will store them in both. Knowing which is the case before epileptic surgery is essential for gauging risk: Will surgery take place in the same hemisphere as these vital cognitive tools?
“I want to be seizure-free and get my life back on track.”
-Ryan MacKenzie
“We perform surgery on dominant brain hemispheres all the time,” said Dr. Antonina Omisade, neuropsychologist with the QEII’s epilepsy care team. “It’s inherently more risky and we need to inform the patient if there’s a likelihood their speech or memory will be affected in some way.”
For this, there’s the Etomidate Speech and Memory test, known commonly as eSAM. Developed at the Montreal Neurological Institute more than a decade ago, eSAM allows physicians to determine exactly this hemispheric dominance. For years this has been the closest facility offering this test; a problematic distance for epilepsy patients unable to drive. Only recently did donated funds from the QEII Foundation allow Dr. Omisade to make the trip, learn the craft and train her team in turn.
“What eSAM entails is the use of an anesthetic to put half of the brain to sleep at a time,” she says. “Once we’ve injected it, only one half of the brain is still operational. At that time we perform a series of language and memory tests to see if the hemisphere awake can support these two faculties independently.”
In this state of half consciousness, Dr. Omisade asks them to name the days of the week, in order, beginning from Wednesday, or the sequence of numbers from 11 to 20. She also asks them to point out and name shapes, to read aloud, and to remember certain objects which she’ll reference once the drug’s worn off.
“Having it here expedites the situations of people who need surgery,” says Dr. Omisade, “and for some unable to travel, it’s the difference between having the surgery and not having it at all.”
Ryan, his epilepsy immune to all the medications he’s been given, was the second Maritimer to experience eSAM at the QEII in March 2018.
“On the second day they put my left hemisphere asleep and asked me to read,” he says. “There were several words I recognized, but I couldn’t say them, no matter how hard I tried.”
This test placed his speech and memory in the opposite hemisphere from the problematic portion of brain being targeted for surgery, meaning the risk is low. A few weeks following his procedure, Ryan had his surgery at the QEII.
“I want to be seizure-free,” he says, “and get my life back on track.”