You are a patient, mentally and physically ready for a scheduled surgery. And sometimes when you’re prepped and waiting, it’s cancelled at the last minute. You’re upset and very frustrated.
The medical staff is no less frustrated but understands, as do most patients fortunately, that cancellations happen for a reason, usually because of emergency, and life-saving, situations.
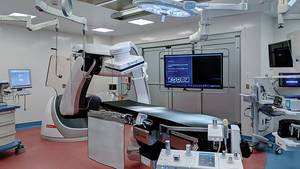
At the QEII Health Sciences Centre, we expect this to happen and plan for it, but from time-to-time, the number of critically ill patients is beyond the norm and saving their lives requires us to cancel surgeries scheduled for non-life threatening conditions.
Every day patients arrive at the QEII Health Sciences Centre with their lives in jeopardy and emergency surgery is the only chance of saving them.
We do our best to let patients know this is always a possibility, yet we know we can do a better job. It starts by explaining the demand emergency surgeries can put on our finite resources.
It’s not just the operating room that is impacted by an emergency. We have to ensure we have an anesthetist and a post-surgery bed. Because of the level of care required, a bed often needs to be located in the intensive care unit or the intermediate care unit.
Other emergency surgeries are organ transplants. There is no way to predict when transplanted organs will become available and, when they do, they can’t be passed up. Patients awaiting transplants may not always be critically ill, but without a replacement organ, they will be. Matching organs are hard to find – some patients wait years – and we only have hours to perform the transplant because tissue begins to deteriorate as soon as it is harvested.
One organ donor may result in as many as four transplantation surgeries – liver, two kidneys, or kidney/pancreas and heart – meaning four ORs must be found. The surgery itself may require a team of up to seven or more.
In an ideal world, we would inform patients the night before if their surgery will be cancelled, but it’s impossible to predict the situation even that far in advance. Every evening the surgery coordinator, anesthetist and charge nurse at each site of the QEII (VG site and HI site) review the current capacity and the next day’s caseload. This provides an idea of how many cancellations might need to be made, but, with constantly changing patient flow, it’s not an accurate assessment. For example, a patient may become critically ill and needs to be moved into the ICU. That’s why the team waits until the morning to cancel.
We are working with surgeons to put a system in place to notify patients, in advance of their surgery, that there is the possibility of cancellation and to explain why this may occur. Often patients think it is because of a staff shortage. This does occasionally happen, but most often it’s because someone else’s life is on the line.
What’s important to remember is your surgery will soon be rescheduled and by waiting a little longer you’re helping to save a life.