|
| Predict Parkinson’s Group has been in progress since 2008 and is funded until 2017 thanks to Dalhousie University Department of Psychiatry Research Fund. (Anita MacPherson Photography) |
 |
| Dr. John Fisk and Kim Good with part of the Predict Parkinson’s team. (Anita MacPherson Photography) |
The Predict Parkinson’s Group researchers are hopeful diagnosing the disease will someday be as simple as completing a smell test in your doctor’s office.
The study, which has been underway in Halifax since 2008, was the brainchild of Dr. Harold Robertson. An expert in Parkinson’s disease, Robertson was inspired by two studies published in Europe — one study looked at Parkinson’s patients and immediate relatives that found there was a significant statistical risk of developing the neurodegenerative disorder if your mother, father, brother or sister were diagnosed; the second study looked at loss of sense of smell in Parkinson’s patients and MRI changes.
Robertson wanted to bring those two ideas together and called on Kim Good, an expert on the olfactory system with a Ph.D in neuroscience, who is on faculty at Dalhousie University. Both she and Dr. Robertson are now the study’s co-principal investigators.
“About 90 per cent of patients diagnosed have what we call anosmia, which means they cannot smell. That’s been known for quite some time, so the excitement was if we can identify people who have a loss in their sense of smell before they develop Parkinson’s we might be able to identify people at the pre-clinical stages,” explains Good.
The study has several different arms. The first group looked at 20 Parkinson’s patients and 20 control group patients. The study is also examining the same variable in patients in the early stages of Alzheimer’s disease to determine whether smell deficits and other markers are specific to Parkinson’s.
Predict Parkinson’s Group is now in the process of recruiting 1,200 people — 600 who are at-risk or with a first-degree relative with Parkinson’s, and 600 people from the general population between ages 45 and 70.
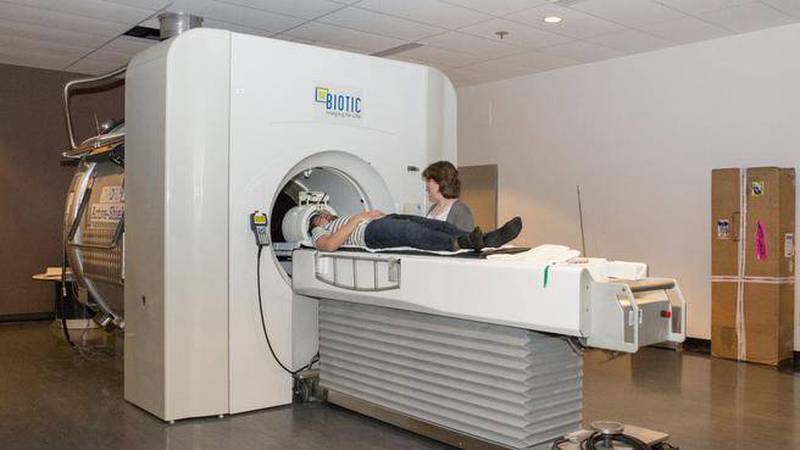
Candidates are sent an at-home scratch n’ sniff test. From there, the top and bottom performers are selected for further cognitive testing, an MRI scan and a sleep study.
Part of the sleep component of the study follows patients recently diagnosed with REM Behaviour Disorder, a sleep disorder in which patients act out their dreams. As many as 80 per cent of patients with REM rapidly develop Parkinson’s within the first few years of their diagnosis.
Thanks to funding from the Canadian Institutes of Health Research, the Parkinson’s Society of Canada and the Dalhousie University Department of Psychiatry Research Fund, the study is funded until 2017 with plans to continue to follow the group for five years after that.
“Most people, because they have a relative and they’ve watched what happened to those people, are very motivated to take part. Many of the healthy subjects in the study are spouses of the affected individuals. Because of this, they are very willing to take part,” says Good. “What we know, is for the most part, the earlier people get treated, the better their outcome.”
“If we can identify people who are truly at risk, who are going to develop Parkinson’s disease, then we can start testing new therapies on them to see whether there is the possibility of stopping it in its tracks or at least slowing down the progression.”
Good sees one of the potential outcomes of the study, a simple smell test, that could be part of a physical exam for people in their 50s. Those with low scores could be sent for an MRI scan with the hope that an early diagnosis would make them a candidate for yet-to-be-developed therapies.
One of the investigators on the ground, Dr. John Fisk, a clinical neuropsychologist at the QEII, believes Halifax is uniquely suited for the endeavor.
“We have an integrated approach...that’s one thing we do quite well around here. In Halifax, in the neuroscience community in general we tend to talk to each other more than other places in Canada,” said Dr. Fisk.
Study founder, Harold Robertson, thinks whatever their findings, they will be significant.
“With Parkinson’s disease, of all the central nervous system disorders, we’re closest I think to having a treatment for it. There’s so much more information now out there and we know more things about the treatment of Parkinson’s disease than any other neurological disorder, even Alzheimer’s,” said Robertson.
“Many of the people involved in the study are in the first stages and their disease doesn’t interfere with their daily living at all, they’re still working. So, if we could stop it at the point where they’re diagnosed by a neurologist, it would essentially be the end of Parkinson’s disease.”
The study is still recruiting participants. For more information visit: http://predictparkinsons.com.