The QEII Foundation’s Rehabilitation Program Endowment Fund was created in 1996 to provide annual grants to the QEII's Acquired Brain Injury program, Spinal Cord Injury/Neuro-Rehabilitation program, Musculoskeletal and Amputee program, and the Assistive Technology program.
To help meet the needs of patients, rehabilitation program grants are awarded to staff working at the QEII’s Nova Scotia Rehabilitation and Arthritis Centre to help improve the lives of patients being treated there.
Joanne Comeau, the program manager of the Neurology and Spinal Cord Injury Service, says one of the biggest needs on the fifth floor is an improved method for patients with extremely limited mobility to be independent with some of the basic functions that many take for granted - like being able to call for a nurse, turn on the TV or make a phone call.
“Many of our patients have limited mobility and movements, so they can’t access their environment like most of us can,” says Joanne, who recalls having patients with such limited movement that they have used a baby monitor so these patients are able to call for a nurse when needed. “Patients with limited mobility of their hands can’t push a call bell button to request a nurse but this is the standard way that many facilities are set up.”
Meanwhile, computer technology has moved forward leaps and bounds the last few years, and new computer interfaces are now available. With the help of the rehabilitation program grants, Kim Parker, a rehab engineer with the QEII’s Rehabilitation Centre, will be putting that technology within the reach of patients.
“Accessible call bells for people with physical disabilities are essential and should be in every room,” says Kim.
Kim and Joanne are putting the grant dollars to work building onto a $5,000 Environment Control System that the pair purchased through a QEII Foundation Comfort and Care grant. It can handle touch-screen and voice controls now, but with the most recent grant they’ll be able to add attachments that allow more accessibility.
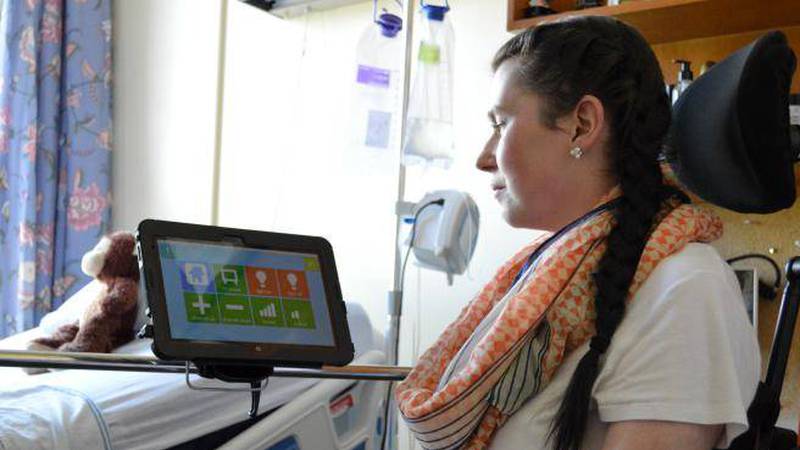
“This is all customizable,” says Kim, who says eye-tracking technology and fibre optic switches - which can cost from $200 to $2,000 - can be attached to the unit and give even highly immobilized patients some ability to control their environments. “Even if someone has only a blink, they can operate the system.”
This system could potentially give patients control over many aspects of their lives, from changing the channel on TV, to making phone calls, and even opening and closing doors.
“This is an excellent opportunity for our patients to be introduced to a system that could be installed in their home. It gives them the opportunity to learn how to use the system and evaluate the potential benefit to their everyday life,” says Kim.
The implementation of the system is in its infancy stage but they’ve been doing trial runs with patients, including Sarah Mather who is temporarily paralyzed from chronic inflammatory demyelinating polyneuropathy (CIDP), a neurological disorder. Sarah, who is unable to do even simple tasks for herself right now, is astounded by the sense of independence it affords her.
“It’s given me freedom of choice. That independence is motivating; I can finally do something for myself,” says Sarah. “That independence makes you feel good as a person.”
Joanne and Kim received funding from the QEII Foundation to purchase technology that will outfit up to four inpatient rooms with increased accessibility. They plan to keep applying for grants each year to build on this technology further.
“The value this adds for our patients cannot be overstated” says Joanne. “This starts to give many of them their independence back and gives them the chance to see that life is possible given their present circumstances.”