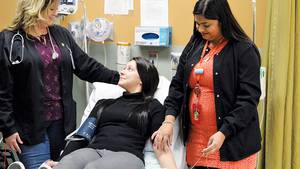
Kellie Williams remembers being called “moody” when she was a teenager. It was not until she reached her mid-20s that she began to experience the true agony of bipolar disorder, with bouts of devastating depression and periods of euphoria.
“I would go on spending sprees and make irrational decisions,” Kellie recalls. “Then when I crashed, I would become extremely depressed and suicidal. It was a very hard time, not knowing from one day to the next how I was going to feel.”
Nine years ago, Kellie was officially diagnosed with bipolar disorder. She was prescribed lamotrigine, and, for a long time, the results seemed promising.
“Within a few short months, everything levelled out,” she says. “I wasn’t suffering depression or mood swings. It was nice, and it lasted for almost six years.”
Then her symptoms returned. It was gradual at first, but she eventually found herself back in the same cycle.
“The depression became severe, and I knew I had to do something fast,” says Kellie.
It was while waiting in a lobby for a mental health assessment that Kellie noticed a poster on a bulletin board. Somebody was looking for volunteers to take part in a study on metabolism and treatment-resistant bipolar depression.
“I called the number right then and there,” she says.
Dr. Cynthia Calkin was spearheading this research. Having practiced family medicine for 10 years before entering the field of psychiatry, Dr. Calkin had unique insight into the mind-body connection in treatment-resistant bipolar depression when she began working in the Mood Disorders Program at the QEII Health Sciences Centre.
“I was seeing patients who were extremely ill and wondering why nobody seemed to be able to make these patients better,” Dr. Calkin says.
She noticed higher than normal rates of obesity in her patient population, along with associated metabolic syndrome, type 2 diabetes, high blood pressure, and high cholesterol.
Insulin resistance is easily overlooked, Dr. Calkin points out, because it is not typically tested for. When she began testing, she found that more than half of her patients were insulin resistant. Studying the case histories of a small number of patients showed that worsening bipolar depression did indeed follow patients becoming insulin resistant.
Considering that insulin resistance appeared to have a big impact on outcomes in bipolar disorder, in 2013 Dr. Calkin founded the Mood and Metabolism Program at the QEII, along with endocrinologist Dr Thomas Ransom.
Beginning in 2016, Dr. Calkin undertook a quadruple-masked, placebo-controlled trial with the drug, metformin, which is used to treat type-2 diabetes.
“We were looking at whether reversing insulin resistance improves outcome,” she recalls. “The patients, on average, had been sick for more than 25 years, with serious impairment in social and occupational functioning. More psychotropic medication was simply not the answer because it was just not working.”
As an endocrinologist, Dr. Thomas Ransom is well versed in the efficacy of metformin, a drug that has been around for more than 75 years.
“It’s a very safe and effective drug, and it has applications beyond treating diabetes,” he points out.
As Dr. Calkin’s colleague at the Mood and Metabolism Program, Dr. Ransom describes his role in the study as a “safety monitor.” He notes that the wider psychiatric community was hesitant, as metformin is not a drug in most psychiatrists’ scope of practice.
“The idea of treating insulin resistance to affect mood is quite new to psychiatry. It can almost seem far-fetched, so that hesitancy was certainly legitimate.”
The resulting study, Treating Insulin Resistance to Improve Outcome in Bipolar Disorder (TRIO-BD), represents an important milestone in the emerging field of metabolic psychiatry. By week six, patients treated with metformin showed significant improvement in depression, anxiety, and overall functioning. They also maintained that improvement throughout the entire 26-week study.
Further research by Dr. Calkin’s team, in collaboration with Dr. Alon Friedman, has provided valuable insights into the blood-brain barrier. Patients with treatment-resistant bipolar disorder have extensive leakage of this barrier, but only in those who are also insulin resistant.
“We know that diabetes causes things to leak – the filter in the kidneys and in the back of the retina — and the damage that this can cause,” Dr. Ransom explains. “The concept of leakage in the blood-brain barrier opens up a whole new area that merits further investigation.”
Being able to apply the results of her research at the Mood and Metabolism Program, and to see an improvement in the lives of her patients, is extremely gratifying, Dr. Calkin says.
“Patients were saying the quality of their remission was different — that this was the best they had felt since before they developed bipolar disorder,” she says.
Kellie says being treated with metformin has been life-altering.
“I was feeling much better, even though we were in the middle of a pandemic. My focus was back, and my work had improved,” recalls Kellie. “I can’t stress enough how much things have changed for the better.
I really believe this saved my life.”
If you have bipolar disorder and are interested in this research or would like to be tested for insulin resistance, contact Claire at 902 943 4753.