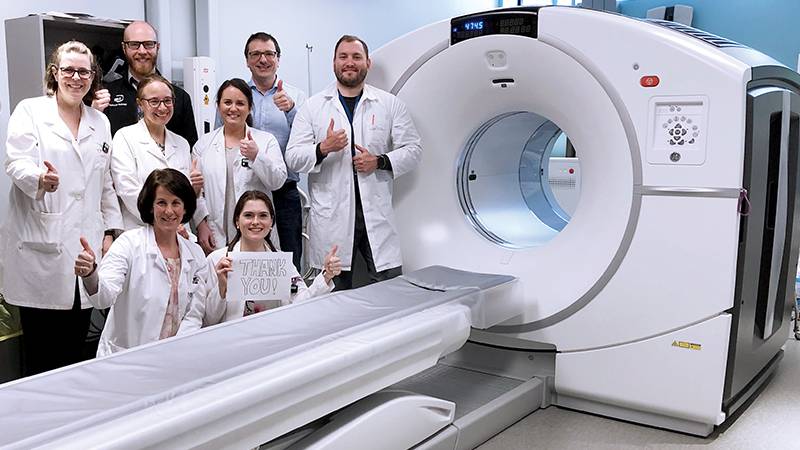
A new PET-CT scanner has increased the number of patients the QEII Health Sciences Centre can see for an important cancer test.
PET-CT combines the technologies of a positron emission tomography (PET) and computerized tomography (CT). While a CT scan provides images of internal organs and tissues, PET shows cellular information to highlight abnormalities in cell function, such as cancer.
More than 1,200 patients have been scanned on the new PET-CT since opening in April 2020 and even the COVID-19 pandemic did not disrupt the new machine’s performance.
For many types of cancers, PET-CT scans are the most accurate imaging test to determine the extent of cancer spread at diagnosis, show the cancer’s response to therapy and identify possible cancer recurrence. A PET-CT scan often finds cancer not seen on other imaging tests and is currently used for the management of more than 2,500 patients every year at the QEII.
The province of Nova Scotia and the QEII Foundation came together to buy the new scanner, dramatically reducing wait times for those in need of this life-saving service.
To inspire community support, QEII radiologists came forward with a $50,000 matching gift — tripling donations to a total impact of $150,000 toward the new scanner.
The new PET-CT has a longer bed, so the entire body can be scanned without moving the patient mid-procedure.
Dr. Steven Burrell, head of nuclear medicine and PET at the QEII, says patients get injected with a radioactive tracer, which is actually just a form of sugar, and most cancers absorb the sugar. When the patients get into the scanner, it detects that tracer and therefore shows the size and location of the cancer. It can also carry out some tests for dementia and heart conditions.
He says the machine looks similar to the old one — at least on the surface.
“They’re now digital detectors, which means they’re much more efficient. There are two advantages to that,” Dr. Burrell says. The first is that instead of about 30 minutes per scan, it takes about 20 minutes. That adds up to three patients per hour instead of two. “That’s extremely helpful because our wait-lists are tight,” he says.
Jennifer Hiltz, a PET-CT technologist, says the process can be an uncomfortable experience for patients. They have to stay calm, breathe steadily and be still, sometimes with their hands stretched over their head.
“Their level of anxiety is already high because they’re either dealing with a new diagnosis of cancer or they’re post-treatment and wondering if it’s worked. The PET-CT test will give them that information,” she says.
“When you’re talking about saving a few minutes here and there on every patient, by the end of the day that works out to scanning more patients than we previously could do.”
The second advantage of the new technology is much better resolution, allowing detection of smaller areas of cancer with greater confidence. This helps ensure cancer patients receive the most appropriate treatment for their cancer situation.
Ami Richardson agrees. She had her PET-CT on the previous machine after a first round of chemotherapy for Hodgkin’s lymphoma, but the images were inconclusive. Faced with the choice between more intensive treatment and waiting and seeing, she chose the latter. It turned out she had to go through another round of treatment.
“If we had had access to that new machine, it probably would have been able to give a much clearer image and decisively say, ‘There’s still some left,’” she says.
The better results and reduced waiting lists are good news for patients, she says. As for herself, she is “doing great” after undergoing more treatment.
The team also devised an innovative way to ensure the PET-CT program at the Health Sciences Centre in St. John’s, N.L., could remain open and operational during the pandemic.
The radioactive substance the PET-CT uses to operate is known as FDG (fluorodeoxyglucose). The QEII uses FDG that is created using a donor-supported cyclotron within the QEII. FDG will decay within a matter of hours, meaning the time spent from production to medical use is limited, making every second critical.
The advanced technology of the new PET-CT requires less FDG to operate than the previous model, meaning the team had additional resources to spare for patients in Newfoundland and Labrador when that province faced a shortage.
This meant Newfoundlanders and Labradorians could continue their care at home and it prevented them from having to fly to Halifax and visit the QEII during the peak of the pandemic — something that would be a risk for any individual, but particularly someone living with cancer.
“When COVID-19 interrupted direct flights from Toronto to St. John’s, the Health Sciences Centre in St. John’s, Newfoundland was unable to reliably acquire FDG, the radioactive substance that a PET-CT uses to operate,” says Brian Martell, the senior director of diagnostic imaging at Nova Scotia Health.
“Sending FDG to the hospital in St. John’s three times a week prevented their program from shutting down and allowed them to continue scanning local cancer patients.”
Without donors, the QEII would not have a best-in-class PET-CT scanner. Cancer patients locally benefit from the most cutting-edge technology when our community rallies to support it.