There was a time when arthritis pain would force John Sperry to stay home.
The retired doctor had always been social and outgoing, but the intense and constant pain in his hip meant he couldn’t stand or walk for extended periods.
There was neither time nor energy for conversations with friends or going for walks — the pain was simply too much.
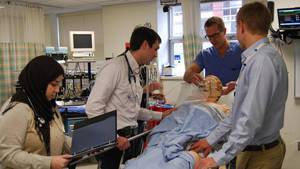
John knew surgery was in his future, but it wasn’t until he was introduced to the QEII Health Sciences Centre’s Orthopaedic Assessment Clinic and Pre-habilitation team that he started to believe in the possibility of an active, pain-free future.
“The last time I had pain was 8 a.m. the morning of my surgery,” says John.
John was part of the very first group of patients who graduated from the QEII’s pre-operative rehabilitation program, also known as pre-hab. Launched in 2019, the program is an eight-week surgery preparation program for patients set to have hip or knee replacement surgery. The program has helped more than 1,000 patients to date.
For the pre-habilitation program, once patients are determined to be a candidate for surgery, members of the multidisciplinary team inform patients about the pre-hab program. If the patient chooses to participate, the team schedules an intake assessment and determines a start date that aligns with their surgery date.
In the weeks leading up to surgery, patients like John attend bi-weekly preparatory classes, which include customized exercise, nutrition, home safety, pain and physiotherapy education and mobility training — like how to safely get in and out of a chair before and after surgery with an arthritic hip.
The Orthopaedic Assessment Clinic team is multidisciplinary — including physiotherapists, nurses, dietitians, social workers, rehabilitation assistants and occupational therapists — ensuring that patients have a holistic plan in place.
“The program was great for setting those healthy habits and talking about goals and mindsets. You could see people improving,” John says, adding that the group setting was a real motivator and source of encouragement.
“We were all there for the same reason, and we all supported each other,” he says.
The program, offered at Orthopaedic Assessment Clinics across Nova Scotia, is among the first of its kind in Canada. It includes 30 minutes of cardio as well as strengthening exercises to target the affected joints.
Dr. William Oxner, the QEII’s chief of orthopaedics, helped lead the team that created the program at the QEII. He says that patient outcomes have been overwhelmingly positive.
“There’s a lot of buy-in for patients to go through the clinic because the rewards are there,” Dr. Oxner says. “We’re trying to create a multidisciplinary approach so that people get more of what they need to help prepare them for surgery.”
In addition to the eight-week program, patients also see healthcare professionals like Michelle Biso, a registered nurse and case manager with the program, for pre-surgery education classes when they are four weeks or less from surgery.
These classes alone have resulted in positive outcomes, with patients arriving on the day of surgery calmer and with a better understanding of what their post-operative care will look like. At home, patients are prepared with mobility aids and the understanding that pain management needs a multi-pronged approach.
“Providing all the instructions up front means that patients aren’t receiving the important information following surgery, when the effects of the anaesthetics are wearing off and the patient is working with the multidisciplinary team to prepare to go home,” Dr. Oxner says.
For Dr. Oxner and the team, filling in some of the gaps of traditional arthritis care was at the heart of the project — and the Orthopaedic Assessment Clinic & Pre-habilitation Program has done just that.
The program plays an important role in helping to increase the number of outpatient surgeries by working with patients and their families or caregivers to ensure they are prepared and have the supports and equipment in place to successfully go home on the day of their surgery. In addition, patients awaiting surgery are getting collaborative, hands-on education on how to manage arthritis and joint pain.
The whole-person approach and focus on a patient’s mental health and well-being is absolutely a success factor for Michelle. She says the results speak for themselves — both before and after surgery.
“Together as a team, a nurse, physiotherapist, occupational therapist, dietician, rehabilitation assistant and social worker wrap ourselves around the patient to figure out what they require to get them ready for surgery,” she says. “After eight weeks, we see a big difference in how strong they’ve become and how emotionally ready they are.”
John’s commitment earned him muscles that were stronger six weeks post-op than they had been before surgery. He’s kept up his walking habit and is chatting with his neighbours again — when they recognize him.
“I’d gone from hobbling around, my face screwed up in pain and my head down to getting my 10,000 steps in,” John says. “Six weeks after surgery, they didn’t recognize me.”
To learn more, visit nshealth.ca/content/orthopedic-assessment-clinic-oac.